Preventive Dental Sciences Department, College of Dentistry, Princess
Nourah Bint Abdulrahman University, Riyadh, Saudi Arabia.
Corresponding author email: aaalshami@pnu.edu.sa
Article Publishing History
Received: 10/07/2021
Accepted After Revision: 26/09/2021
Axenfeld Rieger’s syndrome (ARS) is a rare disease causing genome abnormalities, impeding the development of the alveolar process due to disproportionate jaw growth. This case report presents the interdisciplinary management of an 8-year-old child with ARS exhibiting caries, malformed teeth (conical/microdont teeth), infraoccluded primary molars and hypodontia. After liaising with his paediatrician, treatment was carried out under local anaesthesia which included fissure sealants, fillings, upper overdenture and lower resin-bonded bridge. For aesthetics, an upper overdenture was made to correct occlusion and upper lip support, and also fixed resin-bonded bridge on the lower anterior segment. Early diagnosis and an interdisciplinary approach are necessary to provide the best short- and long-term treatment plans, as well as treatment and follow-up for individuals with the syndrome.
Axenfeld Rieger’s Syndrome, Caries, Hypodontia, Oral Rehabilitation
Alshami A. A. Oral Rehabilitation in an Eight Year Child With Rieger’s Syndrome: A 3-Year Follow-Up Case. Biosc.Biotech.Res.Comm. 2021;14(3).
Alshami A. A. Oral Rehabilitation in an Eight Year Child With Rieger’s Syndrome: A 3-Year Follow-Up Case. Biosc.Biotech.Res.Comm. 2021;14(3). Available from: <ahref=”https://bit.ly/3EtIZqD“>https://bit.ly/3EtIZqD</a>
Copyright © This is an Open Access Article distributed under the Terms of the Creative Commons Attribution License (CC-BY). https://creativecommons.org/licenses/by/4.0/, which permits unrestricted use distribution and reproduction in any medium, provided the original author and sources are credited.
INTRODUCTION
Axenfeld Rieger’s syndrome (ARS) is a rare genetic disorder characterized by malformations of the anterior chamber of the eye (gonio dysgenesis) it may be accompanied by craniofacial, a spectrum of dental and somatic anomalies. Its frequency in the general population has been estimated to be 1 per 200,000. When only the eyes are affected, the condition is termed the Rieger anomaly. At present, two different genes encoding transcription factors (PITX2 and FOXC1) are known to cause the alterations observed in the ARS. In addition, at least two genetic loci involve genes that have not yet been characterized (13q14 and 16q24). Furthermore, two other putative genes have been implicated (PAX6 and MAF), (Alward, 2000, Khatri et al., 2019, Gołaszewska et al., 2021, Siddiqui et al., 2021).
This case report aimed to assess the rehabilitation of function and aesthetics, cosmetically improve the appearance of anterior teeth, management of caries primary teeth, monitoring of developing dentition and oral health maintenance and preventive programme.
Case Report: 8- years-old referred by his General Dental Practitioner (GDP) to our hospital regarding missing permanent teeth. T.D had been diagnosed with ARS syndrome, with ventricular septal defect (VSD) which was surgically corrected in his early years. Examination, radiographs and history were carried out. He was diagnosed with caries, malformed teeth (conical / microdont teeth), infraoccluded primary molars and hypodontia.
Due to the complexity of his condition a multidisciplinary hypodontia clinic visit was needed for planning because T.D was being bullied because of the appearance of his teeth. After liaising with his paediatrician, treatment was carried out under LA which included fissure sealants, fillings, upper overdenture and lower resin-bonded bridge. T.D and his twin brother live with a foster family, and at each visit, his social worker was updated with the progress of his treatment.
Patient details: A male patient was involved in this study who has followed up for 30 months. The treatment was started when the patient age was above eight years and followed up till at the age of eleven years. The assessment of pre-treatment is as follows: No history of dental pain or abscesses. However, T.D. was concerned about his appearance and his foster mother mentioned he was being bullied at school due to his missing teeth.
The patient’s relevant medical history was ARS: vision and hearing impairment and ventricular septal defect which was corrected in his early years, Medication: multivitamins, T.D wears hearing aids. The social history was T.D and his twin brother who has the same condition lived with a foster family for the last 4 years and recently they were adopted by the same family and they became the legal guardians.
The dental history was a regular attendee at general dental practitioner (GDP), No history of operative treatment and tooth-brushing twice daily with children toothpaste (unsupervised). The extra-oral clinical examination was defined as Hard tissue: prominent supraorbital ridges, broad nasal bridge and prominent forehead, Maxillary hypoplasia/prognathic profile (Figure 1), thick glasses and hearing aids, soft tissue, TMJ and lymph nodes: nothing abnormal detected and behaviour: positive toward dental treatment (Frankl Scale:3). The intra-oral examination was as follows:
- Teeth presented intra-orally:
- URD, URC, UR1, UL1, URC, URD
- LR6, LRE, LRD, LRC, LLC, LLD, LLE and LL6
- Good oral hygiene, Caries on LLD and LRD, Conical UR1, UL1
- Infraoccluded primary molars (LRE, LRD, LLD, LLE), Hypomineralised permanent molars
Good oral hygiene, no visible plaque deposits on teeth (Simplified plaque index score). Orthodontic Assessment was confirmed as Mixed dentition stage, Midline diastema (6mm space between upper central incisors), molar relationship: right and left crossbite, upper and lower Arch: anterior segment spacing and skeletal: Class III base (Figure 2).
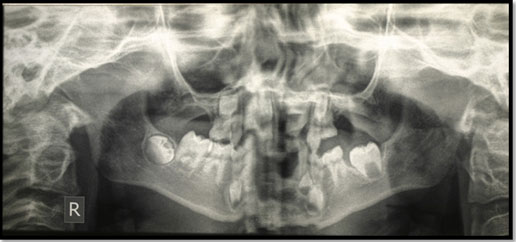
DPT was diagnostically acceptable in the right and left side but not in the middle section presumably because of patient movement. However, caries in primary teeth (LLD, LLE), Infraoccluded (LLD, LLE, LRD and LRE) were found. Also, severe hypodontia (Oligodontia) with upper anterior spacing and skeletal Class III base.
Figure 1: Extra-oral and intra-oral photographs of a patient before the treatment
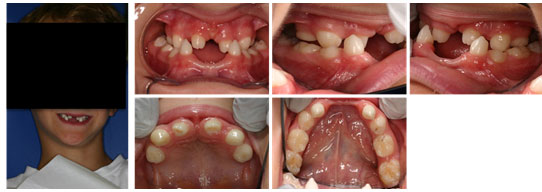
Figure 2: Panoramic radiograph of a patient before treatment
RESULTS AND DISCUSSION
Key stages in treatment progress: T.D.’s physicians were contacted regarding his condition and there were no concerns regarding dental treatment under local anaesthesia (LA). The social worker was contacted and updated regularly with T.D progress. Plaque score 10% and subsequently 0%. The patient was advised to brush twice daily with fluoridated toothpaste that contains at least 1,350 ppm fluoride, and brush at night before sleeping and in the morning. The patient was issued a diet sheet: sweets should be consumed at mealtimes as a dessert rather than between meals. Sugars should not be consumed more than four times per day. Fluoride varnish application on teeth was also advised (2.26% F).
Non-pharmacological behaviour management techniques including tell-show-do and positive reinforcement were used during the provision of preventive care. Local anaesthetic (a pharmacological behaviour management technique) was utilised to provide the planned comprehensive dental treatment (Infiltration of 2% lignocaine with 1:80,000 epinephrine). Treatment performed under LA and rubber dam: Occlusal composite restoration for LLD and LLE
And resin fissure sealant of LRD, LRE, LR6, LLE, LL6, UR1 and UL1. For aesthetics, an upper overdenture was made to correct occlusion and upper lip support and also fixed resin-bonded bridge on the lower anterior segment.Periodic reviews every 6 months were done over 3 years, they involved monitoring of restorations, enhance oral hygiene, eruption pattern of permanent dentition, monitoring infraoccluded primary molars, preventive and dietary advice, and fluoride varnish application with 2.26% (Figure 3).
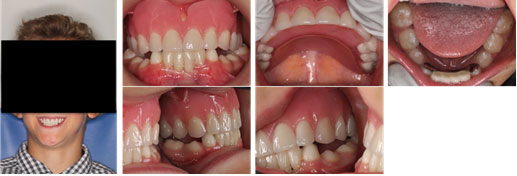
Figure 3: Extra-oral and intra-oral photographs of a patient after the treatment
Congenital heart defects are common in this syndrome and are often the clinical manifestations leading to diagnosis. Many different defects can occur but the most frequently reported cardiac malformations include ventricular septal defect(Alward, 2000).Dental problems are hypoplasia or hypomineralisation of enamel, this common defect can increase the risk for dental caries (as is the case with T.D.). Other dental problems including delayed tooth eruption and aberrant tooth shape, hence close monitoring of the development of the occlusion and radiographic examination should be undertaken at an appropriate age to exclude hypodontia(Brooks et al., 1989, Fitch and Kaback, 1978, Gołaszewska et al 2021).
Several non-pharmacological behaviour management techniques like tell-show-do and positive reinforcement were used with the patient during the preventive care visits aiming to create a positive dental attitude and long-term interest in prevention and maintaining oral health(Silva et al., 2021). T.D’s hearing and vision impairment made communication challenging; however, improvement in his general behaviour toward dentistry was noticed over subsequent visits, his rating on Frankl scale improved positively. However, T.D. was shy and withdrawn during the first few visits, he refused photographs to be taken but subsequently agreed.
Management of hypodontia requires multi-disciplinary care which involves the close working relationship of a committed team contributing their expertise to achieve an optimum outcome for the patient and family. Early orthodontic and restorative interception is highly recommended for the best long-term treatment planning. After referring T.D. to the hypodontia clinic, construction of maxillary overdenture was recommended. This was to improve aesthetics and provide better lip support than ordinary removable partial denture (RPD), (Jepson et al., 2003 Silva et al 2021). In addition, a resin-bonded bridge was constructed for the lower anterior segment instead of RPD as children often cope better with fixed appliances rather than removable especially in the lower arch. Retention of primary molar teeth where the permanent successor is absent is important in cases of hypodontia since they retain bone in an area that may be a site for future transplantation or implant therapy. The prevalence of infraocclusion is 1-9%. Altered pulp pathology determines the most appropriate management but may involve pulp therapy and restoration with pre-formed metal crowns.
Where restoration for caries is not necessary, an infraoccluded tooth that is static may have onlays placed in order to facilitate cleaning as well as preventing food packing and its squeal. If seen early enough it may be prudent, in conjunction with orthodontists, to remove the primary molar tooth where there is no successor to achieve an optimum outcome. The longevity of the primary dentition, where there are no permanent successors, is uncertain, (Nunn et al., 2003, Silva et al 2021). In this case, over the review period, the infraoccluded teeth were at the same level without any signs of ankyloses. Therefore, the suggested treatment was to monitor.T.D had multiple carious lesions with hypomineralisation enamel defects. Therefore, it was important to establish a preventive regimen aiming to prevent the progress of the disease and reduce the risk of the development of further caries.
An evidence-based preventive approach was utilised for T.D. He was placed on 6 months’ recall visits, and with the implementation of behaviour management techniques, he received diet advice, oral hygiene instructions, and fluoride therapy, (Gregory, 2014, Gołaszewska et al 2021).
CONCLUSION
Careful planning of treatment while liaising with other colleagues is essential for the successful management of children with Axenfeld Rieger’s syndrome. This requires clear pre-treatment and early liaising with orthodontics and prosthodontics in the hypodontia clinic.
ACKNOWLEDGEMENT
This research project was funded by the Deanship of Scientific Research, Princess Nourah bint Abdulrahman University, Riyadh, Saudi Arabia through the Fast-Track Research funding programme.
Case Report (Human Studies) Ethical Clearance Statement: The Current Case Report/ Studies were Conducted as Per the Guidelines of SCARE.
Riaz A Agha et al., (2020). The SCARE 2020 Guideline: Updating Consensus Surgical Case Report (SCARE) Guidelines. doi: 10.1016/j.ijsu.2020.10.034. Epub 2020 Nov 9.
REFERENCES
Alward, W. L. (2000). Axenfeld-Rieger Syndrome In The Age Of Molecular Genetics. American Journal Of Ophthalmology, 130, 107-115.
Brooks, J. K., Coccaro Jr, P. J. & Zarbin, M. A. (1989). The Rieger Anomaly Concomitant With Multiple Dental, Craniofacial, And Somatic Midline Anomalies And Short Stature. Oral Surgery, Oral Medicine, Oral Pathology, 68, 717-724.
Fitch, N. & Kaback, M. (1978). The Axenfeld Syndrome And The Rieger Syndrome. Journal Of Medical Genetics, 15, 30-34.
Gołaszewska, K., Dub, N., Saeed, E., Mariak, Z. & Konopińska, J. (2021). Axenfeld‐Rieger Syndrome Combined With A Foveal Anomaly In A Three‐Generation Family: A Case Report. Bmc Ophthalmology, 21, 1-7.
Gregory, S. (2014). Delivering Better Oral Health: What The Third Edition Offers. Dental Nursing, 10, 682-686.
Jepson, N., Nohl, F., Carter, N., Gillgrass, T., Meechan, J., Hobson, R. & Nunn, J. (2003). The Interdisciplinary Management Of Hypodontia: Restorative Dentistry. British Dental Journal, 194, 299-304.
Khatri, A., Beniwal, P., Kalra, N. & Tyagi, R. (2019). Dental And Craniofacial Anomalies Associated With Axenfeld–Rieger Syndrome. Saudi Journal Of Oral Sciences, 6, 41.
Nunn, J., Carter, N., Gillgrass, T., Hobson, R., Jepson, N., Meechan, J. & Nohl, F. (2003). The Interdisciplinary Management Of Hypodontia: Background And Role Of Paediatric Dentistry. British Dental Journal, 194, 245-251.
Siddiqui, H. P., Sennimalai, K., Samrit, V. D., Duggal, R. & Yadav, R. (2021). Adjunctive Orthodontic Therapy For Prosthetic Rehabilitation In A Growing Child With Axenfeld‐Rieger Syndrome: A Case Report. Special Care In Dentistry, 41, 423-430.
Silva, M. V. D., Bussadori, S. K., Santos, E. M. & Rezende, K. M. (2021). Behaviour Management Of The Contemporary Child In Paediatric Dentistry: An Overview Of The Research. Pesquisa Brasileira Em Odontopediatria E Clínica Integrada, 21.


