Department of English and Languages, Amrita Viswa Vidyapeetham, Kochi Campus, India.
Corresponding author email: bincybaby52@gmail.com
Article Publishing History
Received: 18/04/2021
Accepted After Revision: 19/06/2021
Maternal wellbeing is a pivotal subject because it involves both mother and child’s health. But in most cases after giving birth to their young ones, these mothers carry the psychological brunt of being body-shamed leading to body dissatisfaction, depression, and low self-esteem. Nowadays women are given too much pressure to adhere to the standards laid by society which itself proclaims the significance of this study. They are endorsed with the additional responsibility of getting back to their pre-baby body at the earliest. Methodologically to identify the common psychological impacts of body shaming on new moms a case study of 100 new mothers from Ernakulam, Kerala were conducted after endorsement by the Institutional Human Ethics Committee, using convenience sampling. In the wake of acquiring educated assent, a semi-organized poll was utilized to gather information on self-perception discontentment.
Factors responsible for pressurizing them to regain their pre-baby body were analyzed using different measurement scales. Studies based on these samples show that 81.35%of new mothers are either serious victims of body-shaming or are stuffed with a fearful mindset of being body-shamed during their stressful post-partum period. Development of self-recognition disillusionment was common among all. It was found that segments, for instance, higher BMI, socio-cultural strains, and sadness were all basically associated with self-observation frustration. Normally used weight control measures were eating little meals and some even practice skipping dinners83% of women eat less during the lactating period to reduce their prenatal weight gain. Enhancing the appearance and body shape where the essential clarifications behind weight control rehearses. Women undergo physical as well as mental pressures from different walks of life to work for physical perfection, no matter what stage of life they are in now; meeting these societal expectations became the top priority for modern women which acts harmful for a healthy life.
Body Dissatisfaction, Body Shaming, Depression, Maternal Health, Post-Partum.
Baby B.M, Kalamullathil B. Body-Shaming and its Trepidation on the Postpartum Condition of Women: A Psychological Study. Biosc.Biotech.Res.Comm. 2021;14(2).
Baby B.M, Kalamullathil B. Body-Shaming and its Trepidation on the Postpartum Condition of Women: A Psychological Study. Biosc.Biotech.Res.Comm. 2021;14(2). Available from: <ahref=”https://bit.ly/3x6m3sP“>https://bit.ly/3x6m3sP</a>
Copyright © This is an Open Access Article distributed under the Terms of the Creative Commons Attribution License (CC-BY). https://creativecommons.org/licenses/by/4.0/, which permits unrestricted use distribution and reproduction in any medium, provided the original author and sources are credited.
INTRODUCTION
There is a developing contention in our general public, and it’s pointed unequivocally at the waistlines of our moms. No sooner than their nine months of pregnancy are finished, rather than being met with the once standard question about how much their infant’s gauge, moms are being called out about what number of pounds they’ve picked up during their pregnancies and all the more critically, what’s taking them such a long time to lose them. The strain to shed baby blues pounds has brought forth what many propose to be unreasonable assumptions regarding self-perception, blending warmed discussions about how much weight ladies should take on during pregnancy and the worthy measure of time it should take them to get it off. After conceiving an offspring, attaining quick weight reduction has become a mainstream societal fixation, with a-rundown on-screen characters, unscripted television celebrities, and performers continually gracing market tabloids covers, wearing their thinned down post-pregnancy bodies. So, what is the truth about how pregnancy weight gain and loss work? Indeed, a woman’s body is not naturally wired to spring once more into pre-pregnancy shape directly after conveyance. The truth is that it took nine months to get to where you are in terms of weight gain during the pregnancy. It is probably going to take the better part of that to get you back to where you were (Matta 2019).
Many authors have discussed literature based on fat-shaming and its impact on all age groups. Fat shaming and its impact on new moms were not widely discussed, but recently, few articles focusing on these aspects struck my attention. Among them, the most prominent one is the fat studies journal by Taylor and Francis. In comparison to preceding studies, this study base itself on the scientific analysis based on samples of 100 new moms from Ernakulam district of Kerala who contributed their personal experiences making this study unique. Today our culture places too much importance on body weight/size and promotes specific weight gain and weight loss objectives. New moms struggle to get back to their pre-baby body within a short span of time while they are leading a stressful life adjusting themselves with their new ones. The fear of getting body shamed intensifies the psychological stress encountered by them during their post-partum. They even forget that they are lactating mothers; therefore, their body requires sufficient nutrients (Zielinski 2019).
As indicated by Body Mass Index (BMI) rules given by The American College of Obstetrics and Gynecologists and refreshed by the Institute of Medicine in 2009, underweight ladies, with a BMI underneath 18.5, should pick up between 28-40 pounds through the span of their pregnancy; the individuals who have the typical weight (BMI between 18.5-24.9) are supposed to pick-up 25-35 pounds during their pregnancy; overweight ladies with the (BMI between 25-29.9) are only supposed to gain 15-25 pounds during their pregnancy, and large ladies with a BMI of 30 and above are encouraged only to increase 11-20 pounds during pregnancy (Lee 2019). Each individual body is unique and they metabolize differently. Some people gain or lose bodyweight due to certain underlying medical conditions. For instance, patients with thyroid malady or other clinical issues may have various issues with weight (Lee 2019).
There are many works based on fat-shaming and postpartum condition of women but there was a lacuna in studying the impacts of fat-shaming on new moms. Thus, this work concentrated on the scientific study of the psychological impact of body-shaming on the post-partum condition of new moms. During the pregnancy tenure, only very few women happily embrace their weight gain. Most women live in a cocoon of fear of being body-shamed or being compared to those women who have attained their normal body size after few months of their delivery. To put it plainly, persistence rules about how soon ladies can hope to see changes in their post-child bodies. For nursing moms, a twofold portion of persistence is fundamental. At the point when the bosom is taking care of, you’re going to require some additional bodyweight, muscle to fat ratio to take into consideration ideal nursing. The accentuation (for moms) ought to be on keeping up a solid eating routine and a sound way of life, both during pregnancy and a while later, realizing that proper weight gain or loss will follow (Saarikko et al. 2021).
MATERIAL AND METHODS
A case study of 100 new mothers from the Ernakulam district of Kerala was conducted. There was an estimated commonness of body image dissatisfaction and fear of being body-shamed among 81.35% of the study participants. After endorsement from Institutional Human Ethics Committee and acquiring ethical clearance, 100 new moms were taken for investigation by the convenience sampling. In the wake of acquiring educated assent, a semi-organized poll was utilized to gather information on self-perception discontentment among new moms.
They even live in fear of what others will think of them. All these concerns add to the post-partum condition encountered by most women all over the world. It was found that new moms are under the grip of certain unavoidable factors that encircle them like socio-cultural pressure, financial and media impact, statistic factors, blind belief in maintaining normal body size acquired from various spheres of life, and how does it directly affect one’s confidence, out of the box body sizes may even lead to compulsiveness and depression in certain situations. Self-perception discontentment among new mothers was estimated using the Stunkard scale or the Figure Rating Scale (FRS). Females who were under the study were given the adaptations of the FRS and were approached to distinguish the figure they as of now saw themselves with, and the figure they would wish to have. Inconsistency scores were determined dependent on the contrast between the genuine and perfect figures picked. Positive scores demonstrate a longing to be littler, while negative scores recommend a craving to be bigger (Lee 2019).
The disparities between the present and wanted figures were translated as a sign of self-perception discontentment. Thus, members who had disparities in the figures picked were distinguished as having self-perception discontentment. For example, the variables related to self-perception discontentment, confidence, discouragement, socio-cultural pressure, media impact, and perfectionism were estimated utilizing recently approved surveys and utilizing Likert scale evaluations, and a score was given (Lee 2019). Rosenberg Self-Esteem Scale was utilized to quantify Self-regard with the Likert scales running from firmly concur (score 0) to unequivocally dissent (score 3) (Gray1997). Based on the responses from the questionnaire (carrying ten questions), individual scores were calculated with the total score ranging from (0-30). Those who secured (25-30) individual scores were considered to possess a higher level of confidence and higher self-esteem; only 5% secured this score (Lee 2019).
Among them, 80% secured (15-25), indicating that their confidence level was not affected. But 15% of them secured (0-15), which indicated low self-esteem and lack of confidence, which is quite 3) (was estimated utilizing the Center of Epidemiological investigations (CES)with the help of 20 questions. Depression survey was conducted with Likert scale which evaluated from once in a while to generally with the scoring of 0-3, separately (Radloff 1977). Based on the analysis, 40% of the samples secured a score of 45-60, which indicated a higher degree of depressive symptoms, 30% got scoring30-45, indicating mild symptoms of depression. 20% secured 15-30, which is a normal range. Only 10% got 0-15 indicating no or very fewer depressive symptoms. The socio-cultural measure was estimated using SATAQ 4 with scores ranging 1to 5(Thompson 2004). The questionnaire consisted of 3 sections. The first section carries 10 questions with scores (10-50) that calculated individuals’ body image perception (Zielinski 2019).
Accordingly,62.225% preferred thin/low body fat; 19.125% preferred muscular/athletic body; only18.65%was satisfied with their present body image. The following four questions measured the influence of an individual’s family on forming his body image perception.75% of them got15-20, which indicated high level of influence. The next four questions are targeted to measure the peer influence. 81% agree that they are under the strong grip of their peer influence (Zielinski 2019). Media impact was estimated utilizing SATAQ 3surveys with a Likert scale evaluated with a scoring of 1-5. Four questions were targeted to extract the influence of media, and scores of 92.5% cases show that they are under the strong influence of media. Compulsiveness was estimated utilizing the EDI (Eating Disorder Inventory poll) with Likert scale evaluated on the basis of a questionnaire carrying 25 questions with a score ranging from (1 to 6) (Garner 1983). Studies show that 83% of the cases are victims of some sort of an eating disorder.
Among them 61% eat less than the required food to reduce their present body weight; 21% even skip dinner for the same reason. Extraordinary estimates like taking purgatives (17%) and vomiting after dinner (1%) were also observed. The tallness and weight of the members were estimated, and the weight list (BMI) was determined. According to determined. According, BMI<18.5 kg/m2 was named underweight, a BMI of 18.5–24.9 kg/m2 was viewed as typical, overweight is 25–29.9 kg/m2, and stoutness is ≥30 kg/m2 (Saarikko et al. 2021).
RESULTS AND DISCUSSION
Table 1. Body image dissatisfaction and its distribution trend among new mothers based on calculated body mass index
| BMI Status (kg) of new mothers | Total Percentage (Based on Body Weight) | Frequency of Body Dissatisfaction | ||
| Increase weight | Reduce weight | Satisfied percentage with the current body weight | ||
| Underweight | 15% | 74.5% | 8.5% | 17% |
| Normal | 30% | 2% | 41% | 57% |
| Overweight | 45% | 0% | 99.5% | 0.5% |
| Obese | 10% | 0% | 99.9% | 0.1% |
In the light of the BMI measurements, 30% of the samples possessed a typical BMI, while 15% were undernourished; 45% were overweight and 10% were large. The investigation indicated that 81.35% of young ladies were disappointed with their self-perception. Table 1 shows the dissemination of self-perception discontentment based on the determined BMI of the members. It shows that 43% of the members with typical BMI were also disappointed with their appearance and wanted to either increase or reduce their body weight. In the underweight class, 74.5% wanted to increase their weight, and 8.5% still wanted to reduce their weight, further demonstrating the growing demand for having a dainty appearance. Higher BMI, higher financial status, sadness, expanded socio social strain to be flimsy, media impact, and low confidence were seen as essentially connected with self-perception discontentment (Saarikko et al. 2021).
Table 2. Distribution of psychological impacts pertaining to weight obsession on new mothers with different BMI scales.
| BMI Status (kg) | Total Number | Psychological health issues(percentage) | Satisfied Psychological Condition |
| Underweight | 15 | 70.5% | 29.5% |
| Normal | 30 | 65% | 35% |
| Overweight | 45 | 99% | 1% |
| Obese | 10 | 99.7% | 0.3% |
Among 100 new mothers who took an interest in the present examination, 71% of them had already attempted some kind of weight control measures because they are under the intense pressure of either being body-shamed or in the grip of a fear of being body shamed. Among the studied cases, 18.65% were satisfied with their present body size/ shape/ weight, but the fact is that 81.35% are developing a shoddy self-perception. Our examination additionally indicated that 65% of them managed to undergo at least one weight control measure. Multiple reasons were given by them, of which 75% gave the reason of improving their physical appearance and body shape as the main reason for going in for weight control measures and 25% said to look better in clothes (Saarikko et al. 2021).
Refraining from sufficient food intake is awful for your psychological and physical wellbeing. Weight variance can also bring a large group of related reactions that can hurt your physical wellbeing. Based on previous studies, it was found that many people feared that body fat has been connected to an expanded danger of cardiovascular sickness, Type 2 diabetes, and hypertension. The mental effect is similarly disturbing. When calorie counters are inclined, it leads to raised cortisol (the pressure hormone). Another investigation found that expanded worry and refraining from sufficient food intake may result in activated gorging (Lee 2019). Studies focusing on postpartum issues and fatness issues are very common, but body-shaming impact during postpartum are not widely discussed. In comparison to previous studies this work focuses on the health consequences of body shaming in new moms. Due to the fear of being body-shamed, most of them resort to some weight control measures. Some even develop severe psychological issues. Ultimately this article highlights contemporary culture’s obsession with body-shaping practices and its harmful impacts on new moms (Saarikko et al.2021).
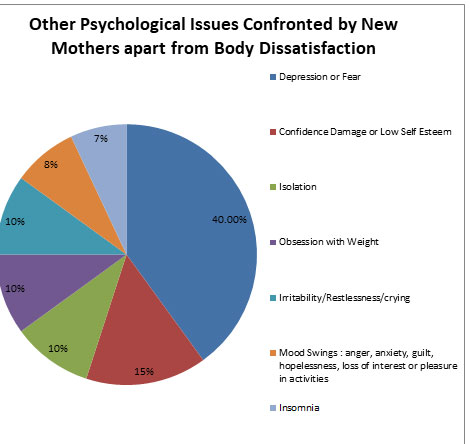
Following pie chart is a pictorial representation of various psychological issues faced by new mothers apart from body dissatisfaction and eating disorders.
Figure 1: Other Psychological Issues confronted Issue confronted by new mothers apart from body dissatisfaction.
CONCLUSION
Body shaming is a powerful strategy asserted with a covert plan of controlling the population and dividing them based on discipline. This explains the growing trend of body shaming. It’s high time to become alert of this victimization and bounce back with the slogan that you are beautiful in whatever size and shape you are in now. Based on this study, it is high time to become alert of the injustice steered on new moms in the form of body-shaming because 81.35% bear the psychological brunt of this cruelty (Rodriguez et al. 2019).
ACKNOWLEDGEMENTS
The study was not supported by any grant’s agency. We acknowledge with gratitude the faculty members of English department in Amrita School of Arts and Sciences, Kochi for providing their generous support and inputs for this study.
Conflict of Interest: All authors contributed equally to this work with no conflicts.
Ethical Clearance Statement: The Current Research Work Was Ethically Approved by the Institutional Review Board (IRB) of Amrita Viswa Vidyapeetham University, Kochi Campus, India.
REFERENCES
Du, Y., (2015). Media Influences on Body Image Dissatisfaction: the Moderating Role of Collectivism vs. Individualism. Journal of Student Research, 4(2), pp.73–87.
Fox, J. (2021). Effects of taking selfies on women’s self-objectification, mood, self-esteem, and social aggression toward female peers. Body Image, 36, pp.193–200.
Garner, D.M. (1982). Eating Attitudes Test-26. PsycTESTS Dataset.
GrayLittle, B., Williams, V.S. and Hancock, T.D., (1997). An Item Response Theory Analysis of the Rosenberg Self-Esteem Scale. Personality and Social Psychology Bulletin, 23(5), pp.443–451.
Lee, J., (2019). You will face discrimination: Fatness, motherhood, and the medical profession. Fat Studies, 9(1), pp.1–16.
Lykins, A.D., Ferris, T. and Graham, C.A., (2014). Body region dissatisfaction predicts attention to body regions on other women. Body Image, 11(4), pp.404–408.
Matta, A., (2020). Weight-Shaming Pregnant Women Affects Their Mental and Physical Well-Being. The Swaddle, Available at: https://theswaddle.com/weight-shaming-pregnant-women-affects-their-mental-and-physical-well-being/ [Accessed May 26, 2021].
Radloff, L.S., (1977). The CES-D Scale. Applied Psychological Measurement, 1(3), pp.385–401.
Rodriguez, A.C.I. (2019). The psychological burden of baby weight: Pregnancy, weight stigma, and maternal health. Social Science & Medicine, 235, p.112401.
Saarikko, J. (2021). Identifying target behaviors for weight management interventions for women who are overweight during pregnancy and the postpartum period: a qualitative study informed by the Behaviour Change Wheel. BMC Pregnancy and Childbirth, 21(1).
Thompson, J.K. (2004). The sociocultural attitudes towards appearance scale-3 (SATAQ-3): Development and validation. International Journal of Eating Disorders, 35(3), pp.293–304.
Zielinski, R.E., (2019). BMI and Pregnancy/Childbirth: Risk Reduction or Fat Shaming?.Women’s Reproductive Health, 6(4), pp.242–244. .


