1College of Nursing, Madras Medical College, Chennai
2Department of Biotechnology & Bioinformatics, Sambalpur University, Odisha
3School of Nursing, Thanjavur Medical College, Thanjavur, Tamil Nadu
4Nurse Educator/Independent Researcher, Chennai
5School of Nursing, Government K.A.P. Medical College, Trichy, Tamil Nadu
6Staff Nurse, NIRT/ICMR, Chennai
Corresponding Author email: shankarshaki@yahoo.com
Article Publishing History
Received: 12/12/2020
Accepted After Revision: 25/03/2021
Globally, the incidence of breast cancer is increasing day by day. In India, it is statistically maintaining an inclination status. The illness’s discomfort initiates stress factors causing emotional instability, aggression, and periods of ups and downs. The impact of coping and social support facilitates quality of life among breast cancer survivors. This descriptive cross-sectional study aimed to explore and analyze the level of stress, coping, and quality of life among 150 breast cancer survivors in Chennai. Socio-demographic and clinical variables were used to assess the baseline data. Stress, coping, and quality of life (QOL) were assessed using a standardized tool like the Perceived stress scale, Hamby, Grych, and Banyard coping scale, and EORTC QLQ – C30 quality life scale, respectively.
The mean age of the participants in this study was 51±9.51years. 77.33% of the participants had a high level of stress. The Coping levels among Breast cancer survivors were 58.67 % (Moderate), and 13.33% (Good). It was reported that 66% of them had a moderate quality of life, and whereas only 20% had a good quality of life. There is a significant, positive, moderate correlation between stress score and coping score (r= 0.56 P=0.001). There was a fair correlation between Stress and Coping with Quality of life. The results revealed that the psychosocial problems among Breast cancer patients were alarming. Necessary screening protocols and health education regarding the management stress, coping strategies are required for the breast cancer survivors, which will help to manage their psychosocial Problems and improve their quality of life.
Breast Cancer Survivors, Coping, Psychosocial, Quality Of Life, Stress
Rajendran S. S, Naik P. K, Venkatesan A, Asaithambi N, Komalavalli, Shankar S. A Descriptive Analysis of the Psychosocial Status of Breast Cancer Survivors from Chennai, India . Biosc.Biotech.Res.Comm. 2021;14(1).
Rajendran S. S, Naik P. K, Venkatesan A, Asaithambi N, Komalavalli, Shankar S. A Descriptive Analysis of the Psychosocial Status of Breast Cancer Survivors from Chennai, India. Biosc.Biotech.Res.Comm. 2021;14(1). Available from: <a href=”https://bit.ly/38soFY6“>https://bit.ly/38soFY6</a>
Copyright © This is an Open Access Article distributed under the Terms of the Creative Commons Attribution License (CC-BY). https://creativecommons.org/licenses/by/4.0/, which permits unrestricted use distribution and reproduction in any medium, provided the original author and sources are credited.
INTRODUCTION
Globally, breast cancer incidence is increasing in the developing world because of increased life expectancy, increase in urbanization, and adaptation of western lifestyle Breast cancer is the commonest cancer diagnosed among women pointing to 1 in 4 cancer cases. Breast cancer is the second frequent cancer and the leading cause of death among women. In 2018, there were 2.1 million new breast cancer cases and 626,679 deaths from breast cancer, in which a large percentage of patients from the low resource sector (UICC 2020). In India, it statistically maintains an inclination status. Moreover, 14% of women, i.e., 1 in 28 females, are affected with breast cancer, and urban women are more affected than rural women (Cytercare 2018, WHO 2021).
Cancer survival is more difficult in higher stages, and 50% of Indian women suffer from the 3rd and fourth stages of cancer. Moreover, new patients’ age group also has gradually fallen from < 55years to below 40years of age. Women’s survival rates are also markedly low in India due to lack of awareness, fewer screening programs, and diagnosed at advanced stages of cancer (Cytercare 2018). Breast cancer diagnosis along with its treatment can direct to physical, social, and psychological turmoil. These difficulties extent to the patients until post-treatment and recovery. The psychosocial impact of breast cancer for a woman is broader, as the breast is the essence of femininity, motherhood, and sexuality (Cytercare 2018; Iddrisu et al. 2020).
In turn, it adds value to their physical appearance, and disfigurement after the surgery creates a loss of self-esteem. The state of disease, the uncertainty of the recurrence in the future, treatment protocols, drug side-effects all these stress factors may lead them to loss of hope, periods of anxiety, impairment of concentration, sleep disorders, mental and cognitive reservation, sexual dysfunction, infertility and fear of death and even depression (Carreira et al. 2018).
Breast cancer is a challenging disease that includes a crisis in psychological balance and is perceived as a disaster in the patient and her family’s view. It develops vast impacts both physically and emotionally. Emotional sensibility and excessive irritability are observed in women diagnosed with breast cancer. The stress factors initiated by the disease process causing emotional instability, aggression, feelings of fear, guilt, and desperation affect their coping ability and quality of life (Hajian et al. 2017; Iddrisu et al. 2020).
The implication of coping mechanism, social support aids in upholding the quality of life of breast cancer survivors. Accompanying psychiatric disorders have a significant impact on a patient’s quality of life, self-care, adaptability to treatment, and over time, the severity and prognosis of cancer and response to treatment. Hence the diagnosis and treatment of psychiatric disorders help in raising the adherence to therapy and quality of life (Izci et al. 2016). The majority of the study analyses found that 50% of the increased risk for breast cancer is due to stressful life in women.
It is found that half of all women with stressful life events are one of the topmost causes of breast cancer in India. The women who experience stress had twice the chance of developing breast cancer than a woman who stays calm and relaxed. That chances of risk double with increased risk factors of breast cancer such as family history, obesity, consuming alcohol, smoking, age of menarche, age of menopause, history of reproductive life, etc (Helgesson 2013; Izci et al. 2016; Iddrisu et al. 2020).
Studies on cellular growth and molecular function stated that due to chronic stress factors, specific pathways originate in cancer growth cells and paves the way for metastasis (Moreno-Smith et al. 2010). Chronic stress creates a perfect storm where pre-cancerous cells can flourish (Parikh et al. 2014). In humans, psychological stress influences the main processes in cancer pathogenesis, such as DNA repair, cellular aging, and alterations in the immune system. The long-lasting biological, psychological, and behavioral changes and have severe effects on health (Krukum et al. 2019).
The prolonged impact of psychological stress causes inflammation and several health problems like anxiety, heart problems, gastrointestinal disturbances, cancer, etc., and incidence of cancer rank topmost among these health problems (Dai et al. 2020). Stress and coping mechanisms among breast cancer patients and family caregivers after breast cancer diagnosis were very high. Coping strategies could either be problem-focused or emotion-focused aids in resolving Stress and increase adaptative coping (Mukwato et al. 2010; Benson 2020).
Coping strategies are specific efforts, both behavioral and psychological, that people use to combat stressful events. It helps to deal with the multi sectoral favorable experiences of psychological, social, and spiritual nature. Coping is behavioral efforts adopted to deal with specific external and internal stressors (Mukwato et al. 2010; Khailli et al. 2013). Coping aids in adaptation and adjustment to breast cancer and enhances the quality of life and survival.
The effectiveness of coping strategies depends on the degree of illness, individual distress, variations in individual coping, the level of social support available, and extended service of consultation skills and support of health personnel (Benson 2020). Quality of life is a state of well-being and the ability to perform daily activities with satisfaction and functioning with control of the disease. Breast cancer patients experience physical symptoms and psychological dysfunctions that adversely affect their quality of life (Sheila et al. 2019).
Clinicians have accepted that survival without complications is the eminent factor for breast cancer patients to enhance their quality of life. Family members play a vital role in breast cancer lives by managing their roles in the family, financial crisis, emotional support, and remaining throughout illness. Hence family support and health-related quality of life lead to improvements in the status of the individual cancer patients and enhance the wellness of the family caregivers.
Therefore, breast cancer is an alarming health problem increasing gradually, the implication of screening protocols and health education among younger women population is essential. Along with a general treatment schedule, standard programs have to be developed to intervene in coping ability to structure their quality of life better, thereby effectively reducing the stress factors (Alexander et al. 2019; Sheila et al. 2019).
MATERIAL AND METHODS
This was a descriptive cross-sectional study conducted among breast cancer survivors. A total of 150 samples were selected by convenient sampling technique. The participants were selected from those attending the Medical Oncology Department, Tamil Nadu Government Multi Super Specialty Hospital, Chennai – 02. The inclusion criteria were a) diagnosed as Breast cancer patients seeking treatment, b) able to understand and speak Tamil c) patients attending the oncology Outpatient and Inpatient department. The study participants were informed about the study in their known language; both oral and written consents were obtained.
The data collection was done with a structured questionnaire consisting of socio-demographic and clinical variables; the perceived stress scale was used to assess the level of stress, coping ability by Hamby, Grych, and Banyard Coping quality of life was assessed using EORTC QLQ -C30 scale. About 20 minutes were spent for each participant to complete the tool. Ethical approval was granted by the Institutional Ethics Committee of Tamil Nadu Govt. Multi-Specialty Hospital vide ref. no. 1577/P&D-I/TNGMSSH/2017/PMS/ 003/07/2020 (Sheila et al. 2019).
The study was also registered with the clinical trial registry of India no. CTRI/2020/08/027291. SPSS software was used for analyzing descriptive and inferential statistics. Descriptive statistics were used in demographic and clinical variables in which categories were given in frequencies with their percentage. Association between demographic variables, coping, and quality of life was interpreted by non – parametric Mann Whitney U test and Kruskal-Wallis H- test.
RESULTS AND DISCUSSION
The study investigated three important psychosocial aspects: stress level, coping ability, and Quality of life of survivors with breast cancer. The socio-demographic variables resulted that the mean age of the participants was 51.57 ±9.51 years (Figure 1), majority of participants were overweight (56.67%), the incidence of breast cancer was high among participants who had primary level education (59.33%), percentage of incidence is high among married women (88%), and participants from the semi-urban region also had higher rate incidence (62.67%). The clinical variables reported that participants who have breast cancer for the past five years were 93.33%, 61.33% were living with III stages of cancer, and 76% slept for 4 to 8 hours.
Figure 1: Histogram with Normal Curve Shows the Age Distribution of Breast Cancer Patients
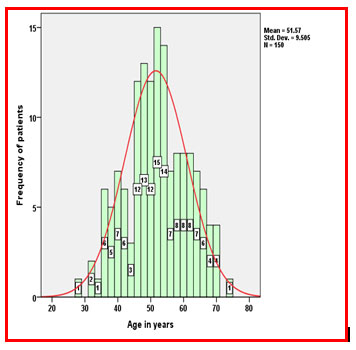
The study results reveal that none of the participants scored a low level of Stress, 22.67% of the participants scored moderate level, and 77.33% were demonstrated a high level of stress score (Table 1). A similar result reported a significant prevalence of Stress among breast cancer survivors and stated that stress factors contribute a significant proportion in increasing the disease process’s severity and reducing the coping skills and Quality of life of breast cancer survivors (Chiriac et al. 2020).
In our study, the association between the socio-demographic profile and Stress reported that Hindu religion participants (P=0.001***), Semi-urban / rural residents (P=0.02*), those who belongs to the nuclear family (P=0.01**), whose cohabitation status were with two and more person (P=0.02*) and those who sleeps less than four hours (P=0.02*) had significant high level of Stress than others. It was also consistent with the study that Stress was commonly prevalent among breast cancer patients among rural residents and those having trouble sleeping and understanding about management aids in the quicker ailment of the patient (Alagizy et al. 2021).
Table 1. Level of Perceived Stress Scale Score
| LEVEL OF SCORE | NO. OF PATIENTS | % |
| Low | 0 | 0.00% |
| Moderate | 34 | 22.67% |
| High | 116 | 77.33% |
| Total | 150 | 100.00% |
The coping ability among Breast cancer survivors was found to be 20% (Good), 58.67% (moderate), and 28 % (Poor) (Figure 2). Participants with a family income of Rs 10,000 (p = 0.05), staying with five or more other persons (p = 0.02), those who were having a recurrence of the breast cancer (p=0.01**), who were partially dependent on others (p=0.01*) and those were sleeping for less than four hours (p=0.01**) gained significant coping score. Similar study also stated that women who perceived proper family functioning were seven more times likely to use active coping strategies (Lopez et al.2018). It is consistent with another study, which reported that family composition and sleeping troubles contribute to the survivors’ coping status (Benson et al. 2019).
Figure 2: Level of Coping Among Breast Cancer Survivors
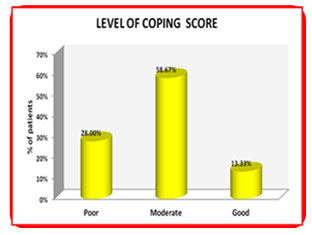
About Quality of life, it was found that 66% of the patients had moderate QOL, 20% of the patients were having good QOL, and 14% of the patients were having poor QOL (Table 2). The association between socio-demographic variables with Quality of life of participants demonstrated a significant association with participants who attained education up to graduation level (p = 0.05*), the participant on II stage of breast cancer (p = 0.001***) and sleeping 4 to 8 hours/day (p=0.001***) were having more QOL score.
The factors affecting the Quality of life in breast cancer patients stress that age, educational status, cancer stage, and status of the disease significantly affect the Quality of life among breast cancer survivors (Sharma et al. 2017). Another study suggested that stages of cancer and educational level were significant predictors of breast cancer survivors’ Quality of life. The tertiary level of education of women had a significant association with Quality of life, and at the early stages of cancer, it is possible to reduce the complications and enhance the Quality of life (Chen et al. 2018).
Table 2. LEVEL OF QUALITY-OF-LIFE SCORE
| Level of QOL score | No. of patients | % |
| Poor | 21 | 14.00% |
| Moderate | 99 | 66.00% |
| Good | 30 | 20.00% |
| Total | 150 | 100.00% |
It was found that there was a positive fair correlation between Stress and coping ability (P≤0.001) (Figure 3). Similar study supported this study, which assesses Stress and coping strategies among women diagnosed with breast cancer. It reported that in situations of Stress aggravated by breast cancer at earlier stages, the patient could adapt and cope with it (Alves et al. 2019).
Figure 3: Scatter Diagram between Stress Score and Coping Score among Breast Cancer Patients.
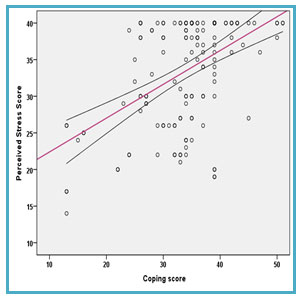
This study conveys the message that psychosocial problems are prevalent among breast cancer survivors, which reflects on the quality of life and recovery. Nurses play a significant role in tackling breast cancer survivors’ psychosocial problems and prolonging the life of the breast cancer survivors in a better way.
CONCLUSION
Breast cancer is the commonest cancer among women worldwide, with an increasing incidence day by day; poverty and illiteracy are the prompt symptoms responsible for delay in seeking medical services. The breast cancer survivors’ psychosocial needs are highly prevalent among them, which need utmost attention at an early stage. Primary prevention aids in the detection of breast cancer survivors at an earlier stage. It also minimizes the severity of illness, enhances the prognosis of health, and reduces the stress factors. In turn, all this develops faith and coping skill in an individual and aids in a better quality of life for cancer breast survivors.
ACKNOWLEDGEMENTS
The Director, Tamil Nadu Government Multi Super Specialty Hospital, Chennai has helped with completing with the research work and finalizing the manuscript.
Ethical Statement: Ethical clearance certificate vide STUDY No : 1577/P&D-I /TNGMSSH/20 l 7/BMS/003/07/2020 dated 22.07.2020
Financial support and Sponsorship: There were no exterior financial support or sponsorship to complete this research.
Conflicts of Interests:The authors declared no conflicts of interest among themselves.
REFERENCES
Alagizy HZ, Soltan M, Solimon SS, Hegazy N, and Gohar N (2020) Anxiety depression and perceived stress among breast cancer, Middle East Psychiatric Journal, Vol 27 No 29 pp 1-10.
Alexander A, Kaluve R, Prabhu JS, Korlimarla A, Srinath BS, Manjunath S, Patil S, Gopinath KS, and Sridhar TS (2019) The impact of breast cancer on the patient and the family in Indian perspective, Indian Journal of Palliative care, Vol 25 No 1 pp.66-72. doi: 10.4103/IJPC.IJPC_158_18.
Alves PC, Santos MCL, and Fernandes AFC (2012) Stress and coping strategies for women diagnosed with breast cancer Brazilian, Journal of Nursing, Vol 13 No 2 pp 305-348.
Benson B (2020) Challenges coping strategies and social support among breast cancer patients in Ghana/Research. Article available at / https: // www. doi.org/10.1155/2020/4817932.
Carreira H, Williams R, Muller M, Harewood R, Stanway S, and Bhaskaran K (2018) Associations between breast cancer survivorship and adverse mental health outcomes: A systemic review, Journal of the National cancer Institute, Vol 110 No 12 pp 1311-1327.
Chen Q, Li S, Wang M, LiuLiu, and Chen G (2018) Health related quality of life among breast cancer patients in eastern china, Biomed research international, available at https: // www. doi.org/10.1155/2018/1452635.
Chirac, Beban A, and Dumitru DL (2020) Psychological stress and breast cancer incidence, Clujan medical journal, Vol 91 No1 pp 18-26.doi: 10.15386/cjmed-924.
Cytecare (2021) Statistics of breast cancer in India /cytecare hospital, https: // www. cytecare.com
Dai S, Mo Y, Wang Y, Xiang B, Liao Q, Zhou M, Li X, Li Y, Xiong W, Li G, Guo C, and Zeng Z (2020) Chronic Stress Promotes Cancer Development, Front Oncol, Vol10.doi: 10.3389/fonc.2020.01492.
Iddrisu M Aziato L, and Dedey F (2020) Psychological and physical effects of breast cancer diagnosis and treatment on young Ghanaian women: a qualitative study, Journal of BMC psychiatry, Vol 20 No 353 pp 1-9.
Hajian S, Mehrabi E, Simbar M, and Houshyari M (2017) Coping Strategies and Experiences in Women with a Primary Breast Cancer Diagnosis, Asian Pacific Journal of Cancer Prevention, Vol 18 issue 1 pp 215-224. doi: 10.22034/APJCP.2017.18.1.215.
Izci F, Ligun AS, Findikli E, and Ozmen V (2016) Psychiatric symptoms and Psychosocial problems in patients with Breast Cancer, Journal of Breast Health, Vol 12 No 94 pp 94-101.
Khailli N, Farajzadegan Z Mokarian F, and Bahrami F (2013) Coping strategies quality of life and pain in women with breast cancer, Iranian journal of Nursing and Midwifery Research, Vol 18 No 12 pp 105-111.
Lopez R, Evelin M, and Cortis M (2018) Family functionality and coping strategies in patient’s health of breast cancer, Journal of Cancer Prevention and current Research, Vol 9 No 5 pp 245-249.
Mukwato K, Mweemba P, Makukula MK, and Makoleka M (2010) Stress and coping mechanism among Breast cancer patients and family caregivers, Medical Journal of Zambia, Vol 37 No1 pp 40-45.
Moreno-Smith M, Lutgendorf K, Anil K, and Sood (2010) Impact of stress on cancer metastasis, Journal of Future oncology, Vol 6 No 12 pp -1863-1881.
Olarewaju S, OyeKunle EO, and Bamiro AO (2019) Effect of socio demographic variables on patient and diagnostic delay of breast cancer at foremost health care institution in Nigeria, Journal of global oncology, Vol 5 No 8 pp-1-6 doi: 10.1200/JGO.19.00108.
Parikh AP, Curtis RE, Kuhn I, Becker-Weimann S, Bissell M, Xing EP, and Wu W (2014) Network analysis of breast cancer progression and reversal, Journal of Plos Computational Biology, Vol 10 No7 pp-1-18.
Rogers LQ, Courneya KS, Oster RA, Anton PM, Robbs RS, Forero A, and McAuley E (2017) Physical activity and sleep quality in breast cancer survivors: a randomized trial, Journal of Medicine and Science in sports and exercises, Vol 49 No10 pp 2009-2015.
Saita E, Acquati C, and Kayser K (2015) Coping with early-stage breast cancer: examining the influence of personality traits and interpersonal closeness, Frontiers for clinical settings, available at; https:// www. doi.org/103389/fpsyg.
Sharma N and Purkayastha A (2017) Factors affecting quality of life in breast cancer patients, Journal of mid-life health, Vol8 No 2 pp 75-83.
Sunday O, Olarewaju EO, Oyekunle, and Adebukola O (2021) A study on effect of sociodemographic variables on patient and diagnostic delay of breast cancer at foremost health care institution in Nigeria, Journal of global oncology, available at https: // www. ascopubs.org/go/authors/open-access.
UICC, (2020) Breast cancer – Thematic areas of work. Union of International cancer control centre. Available at https: // www. uicc.org, thematic areas work.
WHO, (2021) Breast cancer prevention and control, World Health Organization. Available at https: // www. WHO. Int. cancer detection.


