1Basic Dental Science Department, College of Dentistry, Princess Nourah
Bint Abdulrahman University, Riyadh, Saudi Arabia
2College of Dentistry, Princess Nourah Bint Abdulrahman University,
Riyadh, Saudi Arabia
3Ministry of Health, Saudi Arabia
Corresponding author email: ayaloyouny@pnu.edu.sa
Article Publishing History
Received: 15/09/2021
Accepted After Revision: 21/12/2021
Oral hygiene products (OHP) are recommended to maintain the teeth and health of the oral cavity tissues by assisting in lowering the plaque level as well as the opportunistic flora. Oral hygiene products could cause oral health problems that may vary in severity. Due to the availability of over-the-counter (OTC) medications and lack of knowledge, customers may misuse these products. An oral hygiene product is a double-edged sword; a customer would develop side effects from it without even knowing or correlating the source. Many signs and symptoms may appear on the patients such as oral and perioral burning sensations, swelling, erythema, dysgeusia, and dysphagia. To our knowledge and based on the review of English literature through PubMed Midline, this is the first case report of misuse because of an over-the-counter oral hygiene product in which the patient used a mouthwash continuously and aggressively for 15 days without knowing of its side effects.
This case report presents an eighty-two-year-old, male patient who complained of pain, burning, swollen, and dry mouth and lips. The author discussed the most common ingredients of oral mouthwashes. Some active ingredients may irritate the oral mucosa and lips. Also, the author discussed the possible differential diagnosis of painful, sensitive, burning, swollen, and dry mouth and lips. This report is intended as an overview of a rare and unusual oral condition associated with the misuse of OTC oral hygiene products. The findings of the present study necessitated the need for clear verbal and written instructions to be provided to the patients before recommending or prescribing any type of medication.
Atrophic Glossitis; Cheilitis; Dry Burning Mouth; Mucosal Erythema; Mouthwash.
Aloyouny A. Y, Alromaih Y, Alhassoun R. Over-The-Counter Oral Hygiene Products Misuse: A Case Report. Biosc.Biotech.Res.Comm. 2021;14(4).
Aloyouny A. Y, Alromaih Y, Alhassoun R. Over-The-Counter Oral Hygiene Products Misuse: A Case Report. Biosc.Biotech.Res.Comm. 2021;14(4). Available from: <a href=”https://bit.ly/3Cd2BMY“>https://bit.ly/3Cd2BMY</a>
Copyright © This is an Open Access Article distributed under the Terms of the Creative Commons Attribution License (CC-BY) https://creativecommons.org/licenses/by/4.0/, which permits unrestricted use distribution and reproduction in any medium, sources the original author and sources are credited.
INTRODUCTION
Oral care has been an important part of human social life as well as cultural development for hundreds of years. Many OHPs have been invented and produced for the purpose of maintaining good oral hygiene levels. OHPs have been used to control halitosis, dental caries, gingival diseases by lowering the dental plaque and oral bacteria. The accessibility and affordability of OTC oral hygiene products as well as lack of education, explain the misuse of these products (Bourgeois and Llodra 2009). Notwithstanding, OTC oral hygiene products most of the time are safe if used as instructed; however, they have many ingredients that could cause oral irritation if not used properly (Aspinall, Parker and Khutoryanskiy 2021).
The sign and symptoms of acute oral burning, swelling, and erythema are not commonly reported in the literature as side effects of oral hygiene products. Based on a careful review of English literature through PubMed Midline, this is the first case report of misuse because of oral mouthwash in which the patient used the mouthwash continuously and aggressively for 15 days without knowing of its side effects. The lack of knowledge of using OTC products led to acute oral irritation. In this report, the author discusses a case of an eighty-two-year-old man complaining of constant burning and pain in his mouth and lips. After precise exclusion of the diseases and the causative factors, the diagnosis was consistent with acute chemical burn due to misuse of OTC oral hygiene products. “The work has been reported in line with the SCARE criteria” (Agha et al. 2020).
Case Presentation: This case report is about an eighty-two-year-old man, who was referred to an oral medicine clinic to diagnose and manage the patient’s oral condition. He reported a twelve-day history of dry, painful, burning sensations all over the mouth including the lips. He also, mentioned that he felt his lips are chapped and swollen. He could not eat or drink comfortably since he had got that complaint. Also, he mentioned that spicy and sour food had aggravated the burning and pain.
It all started after removing the lower anterior four-unit bridge, he visited a dentist who recommended rinsing with an OTC mouthwash to reduce the intensity and sensitivity of the patient’s exposed lower anterior teeth. The patient reported that he used to swish with 20 mL of an undiluted, mint-flavored mouthwash for four minutes, eight times a day for 15 days. He had diabetes, hypertension, glaucoma, hearing difficulty, and was wheelchair bonded. He was taking metformin 500 mg once per day, lisinopril 10 mg one time per day, and latanoprost 0.005 % once a day before bedtime.
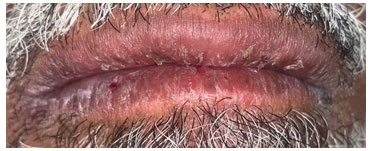
He also denied any changes in his medication list in the last two years. Moreover, he denied a previous history of herpes infection or skin lesions. This also includes a negative history of smoking, alcohol drinking, and drug abuse. The patient revealed that his father had diabetes and passed away due to liver cancer. His mother was healthy, and she died due to a car accident. The oral mucosa and lips were very sensitive to touch that even the slight stretching of the mucosa during examination irritated the patient. Cheilitis was obvious during the extraoral examination which displayed scaly, dry, swollen, and chapped lips (Figure 1).
Figure 1: Extra-oral examination shows scaly, dry, swollen, and chapped lips.
Intraoral examination displayed generalized, diffuse, smooth, bright red, shiny, and edematous buccal and labial mucosae. Additionally, he had gingival and palatal erythema (Figure 2) and atrophic glossitis (Figure 3).
Figure 2: Intraoral examination shows generalized,
smooth, bright red, and shiny gingiva.
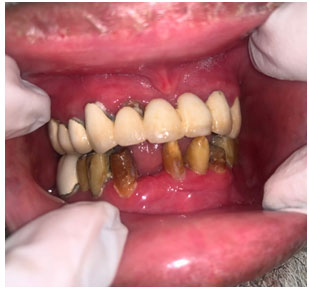
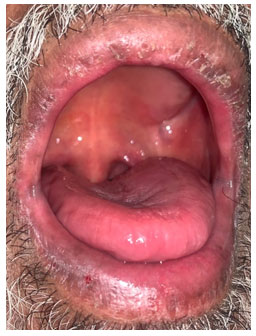
Figure 3: Intraoral examination shows generalized, smooth, bright
red, shiny, and tongue “atrophic glossitis”.
No intraoral vesicles were detected and the Nikolsky test was negative. Regarding the dental concerns, he had multiple missing and carious teeth. Moreover, an old, ill-fitting, porcelain fused to metal (PFM), a 3-unit bridge covering the maxillary edentulous area from tooth number 3 to 5, and a 6-unit bridge covering the maxillary edentulous area from tooth number 6 to 11 (according to the FDI World Dental Federation Notation), and a PFM crown on tooth number 30. A blood sample was collected to detect any systemic problems such as hormonal or nutritional issues; luckily, all blood values showed normal readings. The differential diagnosis included chemical burns, contact stomatitis, cheilitis, microbial infections mainly oral candidiasis, immune-induced lesions including erythema multiforme, nutritional deficiency, and drug-induced oral lesion were all considered. The diagnosis of this condition was made based on the medical and dental history alongside the exclusion of all possible causative factors.
The patient was diagnosed with acute oral chemical burns and cheilitis due to the OTC misuse of the mouthwash. In management, the patient was asked to discontinue the use of OTC mouth rinse instantly. Additionally, he was recommended to avoid spicy and sour food and all flavored oral hygiene products. He was, also, recommended to brush and clean his teeth with baking soda toothpaste gently and to keep away from the gingiva. Therapeutically, topical magic mouthwash was prescribed including viscous lidocaine 2%, diphenhydramine 12.5 mg/5mL, nystatin 100,000 IU, prednisolone 5mg/5mL.
The magic mouthwash is to be used as follows, 5 mL of the solution, swish for two minutes then spit it out, four times per day for 10 days. In addition, for treating the painful cheilitis, the dentist prescribed a mix of clobetasol 0.05% ointment and miconazole 2% to be applied on the lips three times per day for 10 days. The patient came after two weeks for re-evaluation of the oral lesions, the oral mucosae and lips recovered very well with no other complications. Also, he was re-evaluated after one month then two months since the initial visit, he was well and satisfied with the therapy.
Analysis on the case presentation: Oral hygiene products (OHP) are intended to maintain the oral cavity clean and fresh by helping in lowering the plaque level and maintaining healthy gingiva and teeth. Broadly speaking, oral hygiene is ideally performed by mechanical and chemical methods. Mechanical cleaning by using toothbrushes, interdental brushes, dental floss, and dental water flosser. Chemical cleaning by using kinds of toothpaste and mouthwashes. The overuse of OHP products could cause oral mucosal damage that ranges from mild oral irritation and peeling to levels of severe oral mucosal inflammation, ulcerations, and allergic reactions. Ignorance of reading the printed instructions on the OHP packages is the most common cause of OTC-OHP misuse. Also, the availability and accessibility of the OHP on the market/pharmacy shelves make patients think that these products are safe to use regardless of the quantity and frequency (Filipović et al. 2020; Langa et al. 2021).
Mouthwash is a mix of active and inactive ingredients. Active ingredients such as sodium lauryl sulphate (SLS), eucalyptol, menthol, methyl salicylate, fluoride, thymol, peroxide, essential oils, and cetylpyridinium chloride. Inactive ingredients such as alcohol, and benzoic acid. SLS is an active element in many cosmetics and OHPs that works by blending the ingredients. Also, it is considered a foaming agent. Unfortunately, SLS is highly linked to mucosal sensitivity. It was reported that SLS has been associated with oral mucosal inflammation, sloughing, increase chemical-tissue permeability, and alteration of protein structures (Rubright et al. 1978).
Moreover, menthol, eucalyptol, methyl salicylate, cetylpyridinium chloride, and thymol are antimicrobial and antiseptic agents that are widely used in OHP including mouthwashes. In addition, most OHP companies add fluoride to OHP due to its proven effectiveness in reducing dental caries (de Araujo et al. 2012). Peroxide is also used in OHP, specifically in some mouthwashes and kinds of toothpaste that are intended to give teeth a brighter and lighter look (Filipović et al. 2020; Langa et al. 2021).
For more information about peroxide, it is an active content that is also linked to oral irritation and mucosal pigmentation (Aloyouny, Albagieh and Alharthi 2020). Benzoic acid or sodium benzoate is used to increase the lifetime of the OHPs. The differential diagnosis of burning and painful mouth is listed as microbial infection, immunological causes, medications, nutritional factors, and blood disorders. Oral microbial infections are divided into viral, bacterial, and fungal. Viral infections such as herpes stomatitis, herpangina, acute pharyngitis, and cytomegalovirus.
Bacterial infections such as streptococcal pharyngitis or strep throat, and acute necrotizing ulcerative gingivitis or periodontitis (Prieto-Prieto and Calvo 2004; de Araujo et al. 2012). However, the patient in this report did not present with intraoral ulcers, therefore viral infections were excluded. The most common oropharyngeal fungal infection is oral candidiasis that is mainly caused by Candida albicans (Vila et al. 2020).
Painful oral mucosa could be caused by different types of irritations, for instance, traumatic, thermal, and chemical oral irritations. Nutritional deficiency and allergic reactions are proven to cause burning sensations, erythematous and sloughing mucosa, and even ulcerations. Many immunological factors and diseases could induce oral irritation, inflammation, and ulcerations such as lichen planus, erythema multiforme, or in more severe form Steven-Johnson syndrome. Additionally, vesiculobullous diseases such as oral mucous membrane pemphigoid, pemphigus Vulgaris, and paraneoplastic pemphigoid.
However, the patient’s physical examination, in this case, revealed no extraoral or intraoral vesicles, therefore vesiculobullous diseases were not considered. Blood diseases such as acute leukemia could harm the oral tissue appearance and nature (Mortazavi et al. 2016). Luckily, the blood test values in this patient were all within normal limits. In this report, the patient misused the mouthwash as he used it undiluted four times a day for 15 days which caused sloughing of the oral epithelium, dryness, burning, and edema. Mostly, SLS and peroxide, the mouthwash active ingredients caused mucosal tissue irritation (Vila et al. 2020).
On the other hand, with time, all contents of the mouthwash aggravated the oral tissue condition. In case of drug adverse effects or drug misuse, the first line of management is to discontinue the use of the causative agent. It is worth mentioning that in this case, the patient is elderly and had hearing issues. Therefore, the dentist should have to make sure that the patient understood all instructions verbally and should be provided with a written version as well (Vila et al. 2020).
CONCLUSION
The findings of this rare and unusual case of a patient misuse of the OTC mouthwash presented with dryness, burning, and painful erythematous swelling intraorally. Also, chapped, dry, and painful swollen lips. Therefore, thorough instructions should be delivered clearly to patients before recommending or prescribing any type of medication. The patient felt more at ease from the initial visit to the oral medicine clinic. He strictly followed the prescribed therapies. More importantly, the treatment has an excellent impact on his daily routines including eating, drinking, and speaking.
Conflict of Interests: Authors declare no conflicts of interest to disclose.
Data Availability Statement: The database generated and /or analysed during the current study are not publicly available due to privacy, but are available from the corresponding author on reasonable request.
REFERENCES:
Agha, R.A., Borrelli, M.R., Farwana, R., et al. (2020). The SCARE 2020 Guideline: Updating Consensus Surgical CAse REport (SCARE) Guidelines. International journal of surgery (London, England). England, 84, pp. 226–230. doi: 10.1016/j.ijsu.2020.10.034.
Aloyouny, A., Albagieh, H. and Alharthi, S. (2020). Case Report: A rare presentation and diagnosis of gingival melanoacanthoma caused by teeth whitening strips: A Case Report. F1000Research, 9, pp. 1–8. doi: 10.12688/f1000research.27999.2.
ARAUJO, D.B.D., Campos, E.D.J., Bastos, I.H.D.A., et al. (2012). Mouthrinses: active ingredients, pharmacological properties and indications. RGO – Rev Gaúcha Odontol, 60, pp. 349–357. Available at: http://revodonto.bvsalud.org/pdf/rgo/v60n3/a11v60n3.pdf.
Aspinall, S. R., Parker, J. K. and Khutoryanskiy, V. V (2021). Oral care product formulations, properties and challenges. Colloids and surfaces. B, Biointerfaces. Netherlands, 200, p. 111567. doi: 10.1016/j.colsurfb.2021.111567.
Bourgeois, D. M. and Llodra, J. C. (2009). Strategies to promote better access to over the counter products for oral health in Europe: a Delphi survey. International dental journal. England, 59(5), pp. 289–296.
Filipović, G., Stevanović, M.D., Stojanović‐Radić, Z., et al. (2020). Choosing the Right Essential Oil for a Mouthwash: Chemical, Antimicrobial and Cytotoxic Studies. Chemistry & biodiversity. Switzerland, 17(11), p. e2000748. doi: 10.1002/cbdv.202000748.
Langa, G.P.J., Cavagni, J., Muniz, F.W.M.G., et al. (2021). Antiplaque and antigingivitis efficacy of cetylpyridinium chloride with zinc lactate compared with essential oil mouthrinses: Randomized clinical trial. Journal of the American Dental Association (1939). England, 152(2), pp. 105–114. doi: 10.1016/j.adaj.2020.09.021.
Mortazavi, H., Safi, Y., Baharvand, M. et al. (2016). Diagnostic Features of Common Oral Ulcerative Lesions: An Updated Decision Tree. International journal of dentistry, 2016, p. 7278925. doi: 10.1155/2016/7278925.
Prieto-Prieto, J. and Calvo, A. (2004). Microbiological basis of oral infections and sensitivity to antibiotics. Medicina oral, patologia oral y cirugia bucal. Spain, 9 Suppl, pp. 14–15.
Rubright, W.C., Walker, J.A., Karlsson, U.L. et al. (1978). Oral slough caused by dentifrice detergents and aggravated by drugs with antisialic activity. Journal of the American Dental Association (1939). England, 97(2), pp. 215–220. doi: 10.14219/jada.archive.1978.0260.
Vila, T., Sultan, A.S., Montelongo-Jauregui, D. et al. (2020). Oral candidiasis: A disease of opportunity. Journal of Fungi, 6(1), pp. 1–28. doi: 10.3390/jof6010015.


